Operational Obstetrics & Gynecology
Abnormal Bleeding
Normal menstrual bleeding:
- Occurs approximately once a month (every 26 to 35 days).
- Lasts a limited period of time (3 to 7 days).
- May be heavy for pa
- rt of the period, but usually does not involve passage of clots.
- Often is preceded by menstrual cramps, bloating and breast tenderness, although not all women experience these premenstrual symptoms.
Abnormal bleeding (DUB or dysfunctional uterine bleeding) includes:
- Too frequent periods (more often than every 26 days).
- Heavy periods (with passage of large, egg-sized clots).
- Any bleeding at the wrong time, including spotting or pink-tinged vaginal discharge
- Any bleeding lasting longer than 7 days.
- Extremely light periods or no periods at all
Any woman complaining of abnormal vaginal bleeding should of course be examined. Occasionally, you will find a laceration of the vagina, a bleeding lesion, or bleeding from the surface of the cervix due to cervicitis. Much more commonly, you will find bleeding from the uterus coming out of the cervical os.
Excluding pregnancy, there are really only three reasons for abnormal uterine bleeding:
- Mechanical Problems
- Hormonal Problems
- Malignancy
The limited number of possibilities makes your caring for these patients very simple. First, before examining the patient, obtain a pregnancy test. If it is positive, then don't do anything more until you've read about the different possible causes.
Next, obtain a blood count and assess the rate of blood loss to determine how much margin of safety you have. Someone with a good blood count (hematocrit) and minimal rate of blood loss (less than a heavy period), can tolerate this rate of loss for many days to weeks before the bleeding itself becomes a threat.
A variety of pregnancy problems can cause vaginal bleeding. These include:
- Abortion (threatened, incomplete, complete, missed, or inevitable)
- Ectopic Pregnancy
- Placental Abruption
- Placenta Previa
If the bleeding patient has a positive pregnancy test, a careful search should be made for each of these problems. However, if the pregnancy test is negative, pregnancy-related bleeding problems are effectively ruled out.
Read more about Pregnancy Problems
Such problems as uterine fibroids or polyps are examples of mechanical problems inside the uterus.
Since mechanical problems have mechanical solutions, these patients will need surgery of some sort (Polypectomy, D&C, Hysteroscopy, Hysterectomy, Myomectomy, etc.) to resolve their problem.
In the meantime, have them lie still and the bleeding will improve or temporarily go away. Giving hormones (like birth control pills) in an effort to stop the bleeding will not help this condition, but neither will it be harmful.
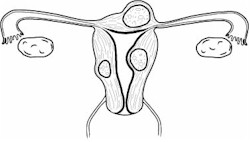 Polyps visible protruding from the cervix are usually coming from the cervix and can be
easily twisted off. However, they will need microscopic evaluation, so removal in many
operational settings may not be desired. Instead, they can await return to a non-deployed
setting.
Polyps visible protruding from the cervix are usually coming from the cervix and can be
easily twisted off. However, they will need microscopic evaluation, so removal in many
operational settings may not be desired. Instead, they can await return to a non-deployed
setting.
Another form of mechanical problem is an IUD causing abnormal bleeding. These should always be removed.
Watch a video on how to remove and IUD
Hormonal causes for abnormal bleeding include anovulation leading to an unstable uterine lining, breakthrough bleeding associated with birth control pills, and spotting at midcycle associated with ovulation. The solution to all of these problems is to take control of the patient hormonally and insist (through the use of BCPs) that she have normal, regular periods.
If the bleeding is light and her blood count good, simply start BCPs (low-dose, monophasic, such as LoOvral or Ortho Novum 1+35 or Ovcon 35, etc.) at the next convenient time. After a month or two, her bleeding should be well under control.
If the bleeding is quite heavy or her blood count not so good, then it is best to have her lie still while you treat with birth control pills. Some gynecologists have used 4 BCPs per day initially to stop the bleeding, and then taper down after several days to three a day, then two a day and then one a day. If you abruptly drop the dosage, you may provoke a menstrual flow, the very thing you didn't want. Giving iron supplements is a good idea (FeSO4 325 mg TID PO or its' equivalent) for anyone who is bleeding heavily.
Abnormal bleeding can also be a symptom of malignancy, from the vagina, cervix or uterus.
Cancer of the vagina is extraordinarily rare and will present with a palpable, visible, bleeding lesion on the vaginal wall. Cancer of the cervix is more common but a normal Pap smear and normal exam will effectively rule that out. Should you find a bleeding lesion in either the vagina or on the cervix, these should be biopsied.
Cancer of the uterus (endometrial carcinoma) occurs most often in the older population (post-menopausal) and is virtually unknown in patients under age 35. For those women with abnormal bleeding over age 40, an endometrial biopsy is a wise precaution during the evaluation and treatment of abnormal bleeding.
Since most (90%) of the non-pregnancy bleeding is due to hormonal causes, and since in operational settings you probably don't have quick access to a D&C, your best bet is to:
- Get a pregnancy test
- Get a blood count
- Examine the patient
- Put the patient to bed if the bleeding is heavy
- Begin BCPs
If this doesn't work, you'll need to MEDEVAC the patient to a definitive care facility, since surgery is the next step for women who do not respond to hormonal control. Obviously, women who are pregnant should not receive BCPs, and pregnant women of more than 20 weeks gestation should be examined vaginally only in a setting in which you are prepared to do an immediate cesarean section should you discover an unsuspected placenta previa.
Heavy periods ("menorrhagia," "hypermenorrhea") and lengthy periods may reflect an underlying mechanical abnormality inside the uterus (fibroids, polyps), may be a cause of iron-deficiency anemia, may contribute to uncomfortable menstrual cramps, and may be a significant inconvenience in an operational setting.If the examination, Pap smear, and pregnancy test are normal, then the chance of malignancy is very low and need not be further considered unless symptoms persist.
One good approach is to give birth control pills to women with these heavy periods. The effect of the BCPs is to reduce the heaviness and duration of flow. If they are anemic, oral iron preparations will usually return their iron stores to normal. If the BCPs (standard, low dose, monophasic pill such as Ortho Novum 1+35, LoOvral or LoEstrin 1.5/30) fail to reduce the flow appreciably, they can be taken continuously, without the usual "week off." This will postpone their menstrual period for as long as several months. Even though their period may still be heavy or lengthy, the fact that they only have it every few months rather than every 4 weeks will have a major impact on their quality of life and anemia, if present. On return to non-operational status, a gynecologic consultation is usually advisable.
Alternatively, you could start the patient on DMPA (depot medroxyprogesterone acetate) 150 mg IM Q 3 months. This will usually disrupt the normal period and she probably won't continue to have heavy periods. There are some significant drawbacks to this approach, however. Light spotting or bleeding are common among women taking DMPA, so you will be substituting one nuisance for another nuisance.
Extremely light periods, so long as they occur at the right time, are not dangerous and really are not a medical problem.
This condition is most often seen among women taking low dose birth control pills. The birth control pills usually act by blocking the normal ovarian function (production of various hormones and ovulation), and then substituting the hormones (estrogen and progestin) found in the BCPs. Usually, the result of this exchange is that the circulating estrogen levels are about the same as if the woman were not taking BCPs. In some women, however, the estrogen levels are significantly lower than before they started taking the BCPs. In this case, they will notice their menstrual periods getting lighter and lighter (over 3 to 6 months), and possibly even disappearing altogether.
This is not dangerous, has no impact on future fertility, and will resolve spontaneously if the BCPs are stopped. Stopping the BCPs is not necessary, however, because there are other safe alternatives. If the periods are simply very light (1-2 days), you can ignore the problem because this situation poses no threat to the patient.
If periods have totally stopped:
- Rule out pregnancy.
- You may change to a different BCP with different hormone in it. This will often lead to recognizable periods because the different hormone is metabolized differently.
- You may add estrogen (Premarin .625 mg or Esterase 1 mg) to each BCP to increase the estrogen stimulation of the uterine lining, increasing its' thickness and leading to heavier periods. After the desired effect has been achieved (recognizable periods), the extra estrogen can be stopped.
- You may safely reassure the patient and allow her to not have periods while taking the BCPs. As long as she otherwise feels well, the absence of periods while taking BCPs is not known to have any adverse effects and some women prefer to avoid monthly flows.
Late for a Period
Pregnancy should be ruled out with a pregnancy test.
If the pregnancy test is negative and the patient is not taking hormonal contraception, then simple observation for a single missed period is the usually the wisest course. Delay of periods in operational settings is common. In Boot Camp, among women not on BCPs, about 1/3 of women will skip periods for up to three months. The same observation is found among college freshman women. Presumably, this is a stress response.
If the patient remains without a period for an extended length of time (3 months or more), then the following are often done:
- Normal menstrual flows are re-established with either BCPs, or Provera (10 mg a day x 5 days, followed 3 days later by a period). Provera works well if ovarian function is not deeply depressed, but will not work for some women. BCPs will usually work regardless of the degree of ovarian suppression.
- The patient is tested for thyroid malfunction. (TSH or Thyroid Stimulating Hormone test).
- The patient is tested for prolactin disorders. (prolactinoma, often associated with inappropriate milk secretion from the nipples)
- The patient is tested for premature ovarian failure. (FSH/follicle stimulating hormone and LH/luteinizing hormone)
If any of these tests are abnormal or neither Provera nor BCPs are effective in restarting normal periods, gynecologic consultation upon return to garrison is indicated.
This means menstrual periods coming at unpredictable intervals, rather than the normal once-a-month cycles.
If the flows, whenever they come, are normal in character and length, this is not a dangerous condition and no treatment or evaluation is required. If the patient finds the irregular character of her periods to be troublesome, then starting low dose BCPs will be very effective in giving her quite normal, once-a-month menstrual flows.
If the flows, whenever they come, are not consistent; are sometimes heavy, are sometimes light, are sometimes only spotting, then they are likely not true menstrual cycles, but are anovulatory bleeding (uterine bleeding occurring in the absence of ovulation). This condition should be treated with re-establishment of normal, regular periods, usually with BCPs. Unresolved anovulatory bleeding may, over many months to years, lead to cosmetic problems (unwanted hair growth due to relative excess of male hormones) and uterine lining problems (endometrial hyperplasia due to a lack of the protective hormone progesterone).
Periods that are too frequent (more often than every 26 days, "metrorrhagia") can be related to several predisposing factors:
- If the periods are otherwise normal, then a short "luteal phase" or insufficient ovarian production of progesterone may be responsible.
- If the periods are inconsistent, then failure to ovulate and the resulting anovulatory bleeding may be responsible.
- If the periods are actually normal and once a month, but there are episodes of bleeding in between the periods, then mechanical factors such as fibroids or polyps may be responsible.
In operational settings, a very good treatment for all of these underlying factors is starting BCPs. On return to garrison, gynecologic consultation is usually indicated to assess the adequacy of symptom suppression and to evaluate the patient for any predisposing, treatable factors.
Women who experience significant daily bleeding for a very long time (weeks) sometimes develop another kind of problem unique to this circumstance, denuding of the uterine lining.
Normally, small breaks or tears in the uterine lining are promptly repaired. For women who have been bleeding for weeks, with the accompanying uterine cramping, the uterine lining becomes very nearly completely lost. There is so little endometrium left that the woman will have difficulty achieving repair and restoration of the normal lining without external assistance. A common example of this situation would be a teenager who has been bleeding for many weeks but who, through embarrassment, has not sought medical attention. On arrival, she continues to bleed small amounts of bright red blood. She is profoundly anemic, with a hemoglobin of 7.0.
These patients do not respond to simple BCP treatment because the BCPs are so weak in estrogen and so strong in progestin that the uterine lining barely has a chance to grow and cover up the denuded, bleeding areas inside the uterus.
These patients need strong doses of plain estrogen, to effectively stimulate the remaining uterine lining (causing it to proliferate). Premarin, 2.5 to 5 mg PO per day, or IV (25 mg slowly over a few hours) will provide this strong stimulus to the uterine lining and if combined with bedrest, will usually slow or stop the bleeding significantly within 24 hours. The estrogen is stimulating the uterine lining to grow lush and thick. The estrogen is continued for several days, but at lower dosages (1.25 to 2.5 mg per day) until the bleeding completely stops. Then, progesterone is added (Provera 5-10 mg PO per day) for 5-10 days. Progesterone is necessary at this point because the lush, thick uterine lining is also very fragile and easily broken. Progesterone provides a structural strength to the uterine lining, making it less likely to tear or break.
Once a normal, thick, well-supported lining has been re-established, first with estrogen, then with the addition of progesterone, it will need to be shed, just like a normal lining is shed once a month. Stopping all medication will trigger a normal menstrual flow about 3 days later. The lining will have been restored and the vicious cycle of bleeding leading to more endometrial loss leading to more bleeding will be broken. Future periods may then be normal, although many physicians will start BCPs at that point to prevent recurrence of the constant bleeding episode.
Hemorrhage is defined differently by different texts, but three good general guidelines are these:
- If the bleeding is heavier than the heaviest menstrual period the patient has ever experienced...that is hemorrhage.
- If, when standing, blood is running down her leg and dripping into her shoes...that is hemorrhage.
- If, because of heavy vaginal bleeding, the patient cannot stand upright without feeling light-headed or dizzy...that is hemorrhage.
Vaginal hemorrhage is more often associated with pregnancy complications such as miscarriage or placental abruption, but certainly can occur in the absence of pregnancy.
This is a true medical emergency and a number of precautionary steps should be taken:
- IV access should be established to facilitate fluid resuscitation
- Blood transfusion should be made readily available, if it proves necessary.
- Pregnancy must be excluded as it's presence may profoundly effect the treatment.
- Bedrest will lead most cases of hemorrhage to slow, regardless of the cause.
- Medical evacuation should be planned as the definitive treatment of uterine hemorrhage not responsive to conservative measures is surgical.
Helpful tips:
- Blood counts (hgb or hct) performed during an acute hemorrhage may be falsely reassuring as the hemoconcentration accompanying hemorrhage may take several hours to re-equilibrate in response to your IV fluids.
- Elevation of the legs to about 45 degrees will add as much as one unit of fresh, whole blood to the patient's circulation by eliminating pooling in the lower extremities.
- In severe cases of hemorrhage when surgical intervention is not immediately available, vaginal packing can slow and sometimes stop bleeding due to vaginal lacerations or uterine bleeding from many causes. After a Foley catheter is inserted in the bladder, a vaginal speculum holds the vaginal walls apart. Tail sponges, long rolls of gauze, 4 X 4's or any other sterile, gauzelike substance can be packed into the vagina. The upper vagina is packed first, with moderate pressure being exerted to insure a tight fit. Then, progressively more packing material is stuffed into the lower vagina, distending the walls. Ultimately, the equivalent of a 12-inch or 16-inch softball sized mass of gauze will be packed into the vagina. This has several effects: 1) any bleeding from the cervix or vagina will have direct compression applied, slowing or stopping the bleeding. 2) The uterus is elevated out of the pelvis by the presence of the vaginal pack, placing the uterine vessels on stretch, slowing blood flow to the uterus and thus slowing or stopping any intrauterine bleeding. 3) By disallowing the egress of blood from the uterus, intrauterine pressure rises to some extent, exerting a tamponade effect on any continuing bleeding within the uterus. Vaginal packing can be left for 1-3 days, and then carefully removed after the bleeding has stopped or stabilized. Sometimes, only half the packing is removed, followed by the other half the following day. The Foley catheter is very important, both to monitor kidney function and to allow the patient to urinate (usually impossible without a Foley with the vaginal packing in place).
Home À Introduction À Medical Support of Women in Field Environments À The Prisoner of War Experience À Routine Care À Pap Smears À Human Papilloma Virus À Contraception À Birth Control Pills À Vulvar Disease À Vaginal Discharge À Abnormal Bleeding À Menstrual Problems À Abdominal Pain À Urination Problems À Menopause À Breast Problems À Sexual Assault À Normal Pregnancy À Abnormal Pregnancy À Normal Labor and Delivery À Problems During Labor and Delivery À Care of the Newborn
|
Bureau of Medicine
and Surgery |
Operational
Obstetrics & Gynecology - 2nd Edition |
This web version of Operational Obstetrics & Gynecology is provided by The Brookside Associates Medical Education Division. It contains original contents from the official US Navy NAVMEDPUB 6300-2C, but has been reformatted for web access and includes advertising and links that were not present in the original version. This web version has not been approved by the Department of the Navy or the Department of Defense. The presence of any advertising on these pages does not constitute an endorsement of that product or service by either the Department of Defense or the Brookside Associates. The Brookside Associates is a private organization, not affiliated with the United States Department of Defense. All material in this version is unclassified.
This formatting ® 2006
Medical Education Division,
Brookside Associates, Ltd.
All rights reserved