|
CORRESPONDENCE
COURSE
U.S. ARMY MEDICAL DEPARTMENT CENTER AND SCHOOL
SUBCOURSE MD0589 EDITION 100
ENVIRONMENTAL INJURIES/DISEASES II
Throughout history, infectious organisms have plagued society.
Biblical accounts of plagues attest to this fact. In London in the
1600s, the Black Plague killed thousands of people.
In a combat situation, the impact of disease on the combat soldier
cannot be overstated. In every war in which the American soldier has
fought, there have been more casualties caused by disease than by
combat wounds. An outbreak of a simple intestinal disease in a combat
zone can greatly affect the morale and fighting strength of the Army.
Information concerning the identification, treatment, and preventive
measures for arthropod-borne, animal-borne, and helminthic diseases
will be discussed in this subcourse. As a Medical NCO, it is extremely
important that you are aware of the prevention and treatments for the
numerous diseases which you will encounter. With the awareness of
those diseases, their general characteristics, modes of transmission,
and clinical findings, you may be alert for either treatment or
prevention.
----------------------
Length: 79 Pages
Estimated Hours to Complete: 7
Format: PDF file
Size: 0.4 MB
----------------------------
Anyone may take this course. However, to receive credit hours, you
must be officially enrolled and complete an examination furnished by
the Nonresident Instruction Branch at Fort Sam Houston, Texas.
Enrollment is normally limited to Department of Defense personnel.
Others may apply for enrollment, but acceptance is not guaranteed.
Environmental Diseases and Injuries II
Distance Learning
Course
79 Pages
Est. 7 Hours
0.4 MB pdf file
Download Now |
|
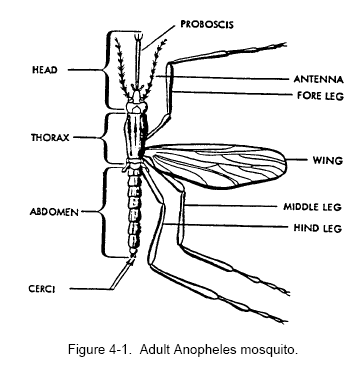
TABLE OF CONTENTS
INTRODUCTION
1 ARTHROPOD-BORNE DISEASES
Section I. Fly-Borne Diseases
Section II. Tick-Borne Diseases
Section III. Louse-Borne Diseases
Section IV. Flea-Borne Diseases
Section V. Mosquito-Borne Diseases
Exercises
2 ANIMAL-BORNE DISEASES
Exercises
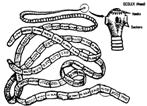
3 HELMINTHIC DISEASES
Section I. Roundworm (Nematode) Diseases
Section II. Tapeworm (Cestode) Diseases
Section III. Fluke (Trematode) Diseases
Exercises
4 MALARIA
Exercises
--------------------------------------
LESSON 1
ARTHROPOD-BORNE DISEASES
Section I. FLY-BORNE DISEASES
1-1. INTRODUCTION
Arthropods are any of the insects, arachnids, or
crustaceans consisting of a jointed body and limbs with the brain
dorsal to the alimentary canal and connected with a ventral chain of
ganglia. The source of the arthropod-borne disease is known as the
reservoir. The vector, usually an arthropod, transmits the causative
organisms of disease to a susceptible person. The organism on which
the parasite lives and from which the parasite obtains its nourishment
is called the host. Autoinfection describes an infection by bacteria
that is present within one's own body.
1-2. GENERAL
a. Transmission.
Diseases are transmitted by houseflies on their hairs and in
their feces and vomitus. Flies breed in manure, human waste, and
decaying organic matter. This decaying organic matter is defined as
the fly's host since it provides the fly with nourishment. Flies
ingest the solid food by vomiting the contents of their stomach onto
the food and then sponging it up.
b. Diseases.
Dysentery, cholera, and typhoid fever are the most important diseases
transmitted by flies.
1-3. DISEASE TRANSMITTED BY FLIES
a. Dysentery.
(1) General. Dysentery is the term applied to a number
of intestinal disorders (especially of the colon) that are
characterized by inflammation of the mucous membranes. It is a common
disease that is often self-limiting and mild but can be serious for
babies up to 3 years old. A rise in strains of dysentery which are
resistant to multiple antibiotics has been noted recently.
(2) Signs and symptoms. Dysentery usually begins
abruptly and the patient has diarrhea, and suffers lower abdominal
cramps and tenesmus. Blood and mucus are often found in the diarrheal
stool. Other symptoms include fever (up to 104ºF in young children),
chills, headache, and lethargy. Meningismus, coma, and convulsions
occur in the most severe cases. Dehydration, weakness, and a tender
abdomen follow as the illness progresses. In infants, dehydration,
acidosis, and electrolyte imbalance occur.
(3) Treatment. The antibiotic of choice is ampicillin
(100 mg/kg/d) which can be given for 5 to 7 days orally in 4 divided
doses. If there is improvement, do not continue with the medication
any longer even if the stool cultures are still positive. Other
medication effectively used in treating dysentery are tetracycline,
chloramphenicol, or co-trimoxazole. Actually the use of even mildly
toxic antibiotics is usually not justified because the majority of
cases are mild and self-limited. For all moderately or severely ill
patients, parenteral hydration and correction of acidosis and
electrolyte disturbances are a necessity. Give clear fluids for 2 or 3
days after the bowel has been at rest for a short time and offer the
patient small frequent feedings with a diet that is soft and easily
digestible. Whole milk, high residue, and fatty foods should be
avoided. If cramps are severe, anti-spasmodics (i.e., tincture of
belladonna) may be helpful. Place the patient on effective stool
isolation precautions to limit the spread of infection.
b. Cholera.
(1) General. Cholera is an acute bacterial diarrheal
disease of the small intestine. Cholera is caused by Vibrio cholerae
which are transmitted by food or drink that is contaminated by feces
containing a large number of vibrios. These vibrios produce a powerful
exotoxin in the small intestine (in particular, the ileum) where they
grow. The reduction of the sodium reabsorption causes massive diarrhea
that is fatal in 50 percent of cases if untreated. This exotoxin
induces hypersecretion of water and chloride in the small bowel.
(2) Signs and symptoms. Cholera victims experience a
sudden onset of painless, watery diarrhea of up to 15 liters per 24
hours. The liquid stool is grayish containing mucus and food
particles. There is no fecal odor, blood, or pus, but rapid
dehydration takes place. The patient may have occurrences of vomiting
and becomes markedly dehydrated and acidotic. His eyes are sunken and
he experiences intense thirst, hypotension, a subnormal temperature,
oliguria, shock, muscle cramps, and coma.
(3) Treatment. The loss of water and electrolyte must
be restored immediately and continuously, and acidosis must be
corrected. Replacement of oral fluids (same volume as that lost) may
be possible in the moderately ill patients. If the patient is unable
to take fluids by mouth, an I.V. infusion of Ringer's lactate must be
used to replace the fluids until the blood pressure and circulating
blood volume are restored. The medication used to suppress vibrio
growth and shorten the time of vibrio excretion is tetracycline, 0.5g
given orally every 6 hours for 3-5 days. If untreated, cholera lasts
3-5 days and has a mortality rate of up to 80 percent. If the victim
receives prompt and competent treatment, however, the mortality rate
can be reduced to 1 percent. The health department must be notified if
it is suspected that a victim has cholera.
(4) Prevention. The cholera vaccine consists of 2
injections of 0.5 and 1 ml. intramuscularly or subcutaneously 1-4
weeks apart, then a booster dose of 0.5 ml is administered every 6
months when cholera is a hazard. Even so, the vaccine offers only
limited protection and has no value in controlling outbreaks. All
water, other drinks, food, and utensils must be boiled or avoided in
endemic areas. When high standards of sanitation and public health
exist, there is rarely an outbreak of cholera of any significant size.
c. Typhoid Fever.
(1) General. The gram-negative rod Salmonella typhi
causes typhoid fever when it enters the victim's gastrointestinal
tract, penetrates the intestinal wall, and produces lesions and
inflammation of the mesenteric lymph nodes, spleen, and small
intestines. The organisms can localize in the kidneys, central nervous
system, the gallbladder, or the lungs with inflammation. The
Salmonella typhi is transmitted by consumption of food or drink
contaminated by food handlers who are healthy carriers. The chronic
carriers with persistent gall-bladder or urinary tract infections are
the main source of most infections.
(2) Signs and symptoms. The onset of typhoid fever is
insidious but can be very abrupt (especially in children) with a sharp
rise in temperature with chills. If untreated, typhoid fever can be
divided into three stages: the prodromal stage, fastigium, and the
stage of defervescence.
(a) Prodromal stage. The victim experiences increasing
malaise, headache, sore throat, diarrhea or constipation, abdominal
pain, vomiting, and the fever ascends in stepladder fashion with each
day's maximum higher than the preceding day.
(b) Fastigium. The fever stabilizes after 7-10 days,
and the victim becomes quite sick. He is motionless and unresponsive,
has half-shut eyes, and appears wasted and exhausted. He has marked
abdominal distention along with "pea soup" diarrhea or severe
constipation.
(c) Stage of defervescence. The victim surviving the
fastigium stage (with its severe toxemia) without complications may
show improvements gradually. His feverish temperature descends to
normal in 7-10 days, and he becomes alert. Relapse may occur as much
as 1-2 weeks after the temperature returns to normal, but the relapse
is usually milder than the original illness. There is a possibility of
having a cardiac arrhythmia. In about 10 percent of the patients, rose
spots (rounded, rosecolored spots that blanch on pressure) appear
between the 7th and 10th day of illness. These spots last from 2 to 5
days and then disappear.
(3) Complications. There are complications in
approximately 30 percent of the untreated cases, and these account for
75 percent of the deaths from typhoid fever. During the third week,
intestinal hemorrhage can occur with a resulting sudden drop in
temperature, sometimes a sudden rise in pulse rate, pallor, sweating,
hypotension, and abdominal pain. Other symptoms of less frequency
include urinary retention, myocarditis, pneumonia, nephritis,
thrombophlebitis, psychosis, cholecystitis, spondylitis (typhoid
spine), and meningitis. Intestinal perforation, the most frequently
fatal complication, is most common during the third week in adult
males. Sharp abdominal pain occurs suddenly (usually in the right
lower quadrant) with nausea, vomiting, fall in temperature, rapid
pulse, and muscle spasm.
(4) Prevention. Typhoid immunization should be
provided for household contacts of a typhoid carrier, for individuals
traveling to endemic area, and during epidemic outbreaks. The vaccine
consists of 2 injections of 0.5 ml each, subcutaneously, 4 weeks
apart. Carriers of typhoid are not permitted to handle food.
(5) Treatment. Administer ampicillin in 4 equal doses
per day, 1 dose every 6 hours for 14 days. Each dose is 25mg/kg.
Another medication for typhoid fever is chloramphenicol, 1 g, which is
given every 6 hours orally or it may be given intravenously until the
fever disappears. After this, give chloramphenicol for 2 weeks at 0.5
g every 6 hours (for children, 50 mg/kg daily). If the infection is
resistant to ampicillin and chloramphenicol, the victim may respond to
trimethoprim-sulfonamide mixtures. The patient should have a
high-calorie, low-residue diet, and his skin must have care. It may be
necessary to administer parenteral fluids in order to supplement oral
intake and maintain urine output. If the patient is severely toxic,
administer hydrocortisone, 100 mg intravenously every 8 hours.
From
Environmental Diseases and Injuries II |


